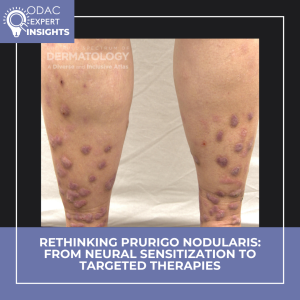
At ODAC 2026, Adam Friedman, MD, FAAD, shared a prurigo nodularis (PN) case that might feel familiar: multiple nodules, relentless itch, one question — why? His message: PN is not merely scratching or a bystander to other dermatoses. It’s a distinct neuroimmune disorder with systemic implications, and overlap does not mean sameness.
PN is sustained by a maladaptive neuroimmune loop: IL‑31 drives itch via sensory neurons, periostin amplifies neural signaling and keratinocyte inflammation, and chronic scratching remodels skin and nerves. Clinically this maps to two meaningful subtypes — inflammatory‑predominant and neuropathic‑predominant — which helps explain variable responses to therapy.
Management goals are simple: reduce itch, interrupt the itch‑scratch cycle, and heal lesions. Tools span topical agents (emerging data for ruxolitinib), neural modulators (gabapentin, pregabalin, mirtazapine), adjuncts like PEA, targeted biologics (nemolizumab), and evolving JAK inhibitors. Expectation setting is key: control, not cure, and “stay on to stay clear” for many patients.
PN often coexists with systemic disease and lifestyle factors that compound burden and reduce quality of life. As mechanism‑driven therapies expand, identifying phenotype and personalizing combinations will improve outcomes.
Read the full session summary, written by Tammy Gonzalez, MD, PhD, to dive into Dr. Friedman’s practical framework and therapeutic insights.
