During the 2020 ODAC Dermatology, Aesthetic and Surgical Conference, Dr. Amy McMichael, Professor and Chair of Dermatology at the Wake Forest University School of Medicine, sat down with Next Steps in Derm to share important updates regarding treatments on the horizon for the most common forms of hair loss. Dr. McMichael will be presenting at Skin of Color Update 2020 with lectures including Hair & Scalp Disorders in SOC: Diagnostic Approaches and Hot Topics & Controversies in Photoprotection: Making sense of it all.
Source: Next Steps in Dermatology
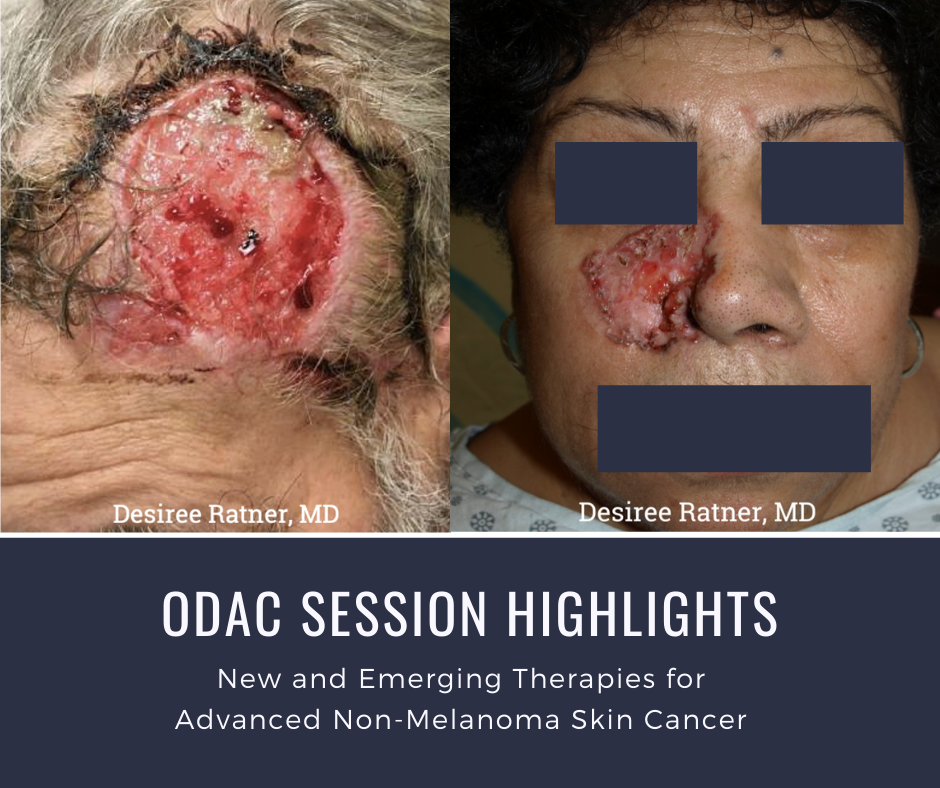
At the 17th Annual ODAC Dermatology, Aesthetic, and Surgical Conference (ODAC) held January 17-20 in Orlando, FL, Dr. Desiree Ratner led a discussion on new and emerging therapies for advanced non-melanoma skin cancer discussion.
Treatment Options
The session covered several treatments for patients including patidegib gel 2% and 4% applied once or twice daily in patients with basal cell carcinoma. Patidegib is a topical hedgehog inhibitor made by PellePharm and its mechanism of action is to block Smo signaling, thereby inhibiting the hedgehog pathway that contributes to the development of basal cell carcinomas. This treatment has several advantages in that it does not contribute to hair loss, taste loss, or muscle cramps. It has the potential to treat and mitigate facial basal cell carcinomas in basal cell nevus patients. It is being studied in randomized clinical trials enrolling patients with Gorlin’s syndrome (basal cell nevus syndrome) in the United States and in Europe.
Hedgehog pathway inhibitor resistance is unusual but may occur as “rebound” tumor growth after drug cessation or secondarily after long-term smoothened inhibitor therapy. Resistance to hedgehog pathway inhibitors is classified into primary and secondary resistance. Primary resistance has been postulated to bypass mechanisms of genes downstream of smoothened, such as the G497 W mutation. Secondary resistance in patients who showed an initial response has actually been thought to be due to de novo mutations located on regions in smoothened to which hedgehog pathway inhibitors bind or selective clonal expansion of minority clones in the pre-treated tumor. Further studies are definitely needed to elucidate what drives resistance to hedgehog pathway inhibitors and how basal cell carcinoma resistance may be overcome by other novel, emerging therapies.
Patient Cases
Dr. Ratner presented a number of interesting patient cases with advanced basal cell carcinomas sometimes so large that patients lose mobility and function of a body part or organ. In most cases, locally advanced BCCs respond well to oral hedgehog inhibitors, which can be used for long-term control or neoadjuvantly prior to surgery. In the case of one patient, an aggressive orbital BCC caused contraction of the tissues around his eye, such that he was not able to open it. Despite treatment with an oral hedgehog inhibitor, his tumor continued to grow, resulting in destruction of his orbit and locoregional metastasis.
Samples of his tumor and normal skin were sent to Stanford University, which performed whole exome sequencing. In the studies of these samples, it became evident that the tumor should have responded to vismodegib but had developed resistance due to another as yet unknown mechanism. Therapies designed to override resistance such as second-generation smoothened inhibitors are under development.

Source: The Dermatologist
The following is an excerpt from The Dermatologist as coverage from ODAC Dermatology, Aesthetic & Surgical 2020 where Sailesh Konda, MD, and Vishal Patel, MD, reviewed the guidelines and discussed considerations for when and when not to perform MMS.
Mohs micrographic surgery (MMS) is considered the gold standard of treatment for many skin cancers. However, this option is not always appropriate for every situation and every patient. Several factors should be considered when determining which option to use, including tumor size, patient age, and aesthetic outcomes, for treating skin cancer.
The Dermatologist: What are the guidelines for determining what tumors should and should not be treated with MMS?
Dr Konda: The appropriate use criteria (AUC) for MMS was developed in 2012 by an ad hoc task force.2 In general, MMS may be considered as a treatment option for tumors on the head, neck, hands, feet, pretibial surface, ankles, and genitalia; aggressive tumors of any location; tumors greater than 2 cm on trunk or extremities; recurrent tumors, and tumors arising in patients with a history of immunosuppression, radiation, or genetic syndromes.
An AUC score is assigned to tumors based on their characteristics. Tumors with scores of 7 to 9 are appropriate, 4 to 6 are uncertain (in extenuating circumstances, MMS may be considered), and 1 to 3 are inappropriate.
However, practitioners should remember that these are only guidelines! Even if a tumor meets criteria for MMS, the physician and patient should still discuss all available treatment options—both surgical and nonsurgical— and take into consideration associated cure rates; long-term clinical and aesthetic outcome; the patient’s age and comorbidities; and risks, benefits, and adverse effects before deciding on a treatment.
The Dermatologist: What tumors often deemed appropriate for MMS might not actually require MMS, and why?
Dr Konda: Superficial basal cell carcinoma and squamous cell carcinoma in situ are tumors that have been deemed appropriate for MMS. However, these tumors may also be treated with topical therapy (imiquimod and 5-fluorouracil), local destruction, fusiform or disc excision, photodynamic therapy, and lasers (CO2 +/- diode for follicular extension). These treatment modalities may provide cure rates lower than but approaching those of MMS, and may be preferred by physicians and patients in certain circumstances. When discussing treatment options, patients should be made aware of any therapies that may be used off-label or are not FDA-approved.
Additionally, lentigo maligna (melanoma in situ) and lentigo maligna melanoma may be treated with either MMS (frozen sections), staged excision with central debulk and complete margin assessment (permanent sections), or wide local excision (permanent sections).

Source: Dermatology News
The following is an excerpt from Dermatology News Expert Analysis, Conference Coverage from ODAC.
ORLANDO – Dermatologists should be well versed in addressing common concerns that patients, family members, and the media have about photoprotection, Adam Friedman, MD, advised at the ODAC Dermatology, Aesthetic, & Surgical Conference.
“Know the controversies. Be armed and ready when these patients come to your office with questions,” Dr. Friedman, professor and interim chair of dermatology at George Washington University, Washington, said in an interview at the meeting, where he presented on issues related to photoprotection.
Which SPF to choose and the impact of sunscreen on vitamin D are among the issues patients may be asking about. Sunscreen SPFs above 50 don’t technically provide a “meaningful” increase in ultraviolet protection, given that this value relates to filtering about 98% of UVB, but they still can provide some benefit, which has to do with real-world human error, Dr. Friedman said.

Source: Dermatology News
The following is an excerpt from Dermatology News Expert Analysis, Conference Coverage from ODAC.
ORLANDO – Because Food and Drug Administration–approved treatment options for children and adolescents with severe dermatologic diseases are limited, systemic therapies for these patients often require the use of off-label medications. However, this scenario is changing, A. Yasmine Kirkorian, MD, said at the ODAC Dermatology, Aesthetic & Surgical Conference.
“I really would like to emphasize that children with severe disease need to be treated,” added Dr. Kirkorian, a pediatric dermatologist at George Washington University, Washington, and Children’s National Health System, where she is interim chief of the division of dermatology.
Current on-label systemic therapies for pediatric skin disease include etanercept for psoriasis (4 years and older), ustekinumab for psoriasis (12 years and older), adalimumab for hidradenitis suppurativa (12 years and older), and omalizumab for chronic idiopathic urticaria (12 years and older). A new addition to the list is dupilumab, which was approved for children and adolescents with atopic dermatitis (AD) aged 12 years and older in 2019, she noted.

Source: The Dermatologist
The following is an excerpt from The Dermatologist article on Q&A with ODAC Dermatology, Aesthetic and Surgical conference faculty, Terrence Keaney, MD.
More and more men are seeking cosmetic procedures to improve their appearance and slow the aging process. In addition to anatomical differences, men have different concerns about how they look compared with women. Terrence Keaney, MD, discussed these concerns and trends among male aesthetic patients, and also shared pearls for treating this patient population at ODAC Dermatology, Aesthetic and Surgical conference in Orlando, FL.
Dr Keaney is founder and director of SkinDC and an assistant clinical professor of dermatology at George Washington University School of Medicine.
The Dermatologist: What are some common trends among male aesthetic patients?
Dr Keaney: Like broader trends in aesthetics, there is no cookie cutter technique for treating men. Gender is just one data point, albeit a fairly important one because it affects biology, anatomy, behavioral expectations, etc. When evaluating a new cosmetic patient, gender, age, ethnicity, and other patient factors play a role in creating a customized treatment plan.
Understanding aesthetic procedures among male patients has not been well-studied and has not been on the top of many aesthetic providers minds, most likely because men occupy a smaller percentage of cosmetic patients. However, the number of men seeking minimally invasive procedures is growing.
As more men seek cosmetic treatment, it is important that physicians and practitioners know how to approach these patients from a treatment perspective, as well as how to discuss complications from these procedures because these scenarios may be different compared with female patients.
The Dermatologist: What are some of the differences between male and female patients that dermatologists should keep in mind?
Dr Keaney: The number one difference between men and women is anatomy. Anatomy really dictates how a provider will perform a procedure, especially fillers.
The facial anatomy of men is very different than women. For example, the distribution of fat is different between the sexes. Men have less subcutaneous fat in the face, especially in the medial cheeks and middle of the cheek, and do not have high cheekbones, which dictates where a filler would be placed. The apex of the cheek tends to be lower and more towards the middle in men, whereas the apex tends to be high and lateral in women and is considered a very feminine feature.
Behaviors, such as goals and expectations of cosmetic procedures, differ between men and women as well. Men care about different factors than women. Specifically, men worry about 3 areas: the hairline, eyeline, and jawline. When discussing aesthetic procedures and performing a full-face analysis of male patients, I often refer back to these 3 areas because I know men tend to worry about them the most.
However, this does not mean I do not use fillers on the cheeks or the mid-face. When I use a filler, I explain to the patient so they understand how this procedure may influence how their jaw looks or their eyes look. Otherwise, they may not be interested in that treatment option.
Other major concerns among men include hair loss and body contouring.

Source: Next Steps in Derm
At the 17th ODAC -Aesthetic, Surgical and Clinical Dermatology Conference held January 17-20, 2020 in Orlando, FL, Dr. Angelo Landriscina led a session on developing new approaches to caring for LGBTQ+ patients.
Next Steps correspondent Dr. Anna Chacon reports back on highlights and pearls from the session which covered the following:
Why this topic?
Updating Our Understanding of SGM Patients
Caring for Transgender Patients
Aesthetic Treatments for Transgender Patients
Creating A Competent Clinical Environment
Why this topic?
It is difficult to determine how many people identify as LGTBQ+ in the United States. Right now, our best estimate is about 4% based on survey data. These patients tend to cluster into different areas, but it’s likely that you will see 2-3 patients per day who are a part of these communities.
Using the appropriate terminology is also key. There is a difference between sexual orientation and gender identity. Sexual orientation describes an individual’s emotional, romantic or sexual attraction to others while gender identity can be male, female or neither, and it can change over time.
What does LGTBQ+ stand for?
The acronym stands for lesbian, gay, bisexual, transgender, queer and questioning but can even be longer (LGBTQQ2SIAA)! There are other terminologies that can also be included such as intersex, gender fluid, and gender queer. Intersex describes: a variation in sex characteristics including chromosomes, gonads, or genitals that do not allow an individual to be distinctly identified as male or female. Gender fluid describes a person who doesn’t identify with a fixed gender at all times. And genderqueer is an umbrella term for gender identities that are not exclusively masculine or feminine identities which are thus outside of the gender binary and cisnormativity.
Queer is a blanket term that can describe all of these but has a loaded history since it used to be use as a slur. SGM stands for sexual and gender minority, which is an easy clinical and scientific term to use when talking about this population. While it is helpful to become familiar with the appropriate terminology, it is also important to be mindful of which particular terms to avoid when talking to patients such as: homosexual, sexual preference, “lifestyle,” and “sex change.”.
When it comes to pronouns, it is best to ask patients which they prefer. In situations where this may be unclear, the singular pronoun “they” may be your best friend – it was Merriam-Webster’s 2019 word of the year!
Additional tips for the dermatologist include being comfortable with not knowing everything, allowing your patients to define themselves, and recognizing that sexual orientation and gender identity are independent of each other.
Source: Next Steps in Derm
Dermoscopy, also known as epiluminescence microscopy, epiluminoscopy or skin surface microscopy, is an important way to visualize subsurface structures in the epidermis and dermis. In a 2-part series, Dr. Sima Jain reviews the evaluation of pigmented lesions, and the different vessel morphologies and patterns along with a discussion of specific findings in select cutaneous infections.
Read part 1 here
Read part 2 here
If you want to learn more about dermoscopy, make sure to register for the upcoming ODAC Dermatology, Aesthetic & Surgical Conference where Dr. Sima Jain will lead the following dermoscopy sessions:
The Utility of Dermoscopy in Challenging Clinical Cases
During this session, Dr. Jain will present challenging clinical cases and explore how dermoscopic evaluation can significantly increase clinical acumen.
Attendees will:
- Learn how to use dermoscopy to help differentiate types of alopecia
- Learn how to use dermoscopic features to differentiate between melanoma and pigmented basal cell carcinoma
- Learn the dermoscopic features seen in cutaneous lupus and other rashes with follicular plugging.
PEARL ALERT!
Perifollicular scaling and fibrotic white dots are seen in lichen planopilaris. Orthogonal white streaks can be seen in melanoma. Glomerular vessels are often seen in Bowen’s disease.
Dermoscopy Essentials for Residents & Practicing Physicians
During this session, Dr. Jain will review the basics of dermoscopy and how it can be used to help diagnose both pigmented and non-pigmented skin lesions.
Attendees will:
- Learn how to correlate the colors seen on dermoscopic exam with histopathology.
- Learn how to distinguish non-melanocytic growths from melanocytic growths.
- Learn how to use vessel morphology to help diagnose cutaneous malignancies.
PEARL ALERT!
White streaks can be seen in melanoma and basal cell carcinoma. Telangiectasias, leaf-like areas and spoke wheel pigmentation are seen in basal cell carcinomas. The delta wing jet with contrail is specific for scabies.

Source: SanovaWorks
NEW YORK – Erik J. Stratman, MD, 2019 President of the American Board of Dermatology (ABD), to present on Maintenance of Certification (MOC) CertLink in January at ODAC Dermatology, Aesthetic and Surgical conference.
Changes to MOC
A major shift in continuing certification is coming for board-certified dermatologists in January. Erik J. Stratman, MD will present, “Changes to Your MOC Requirements: What Every Dermatologist Should Know about CertLink,” on January 17th, 2020 at the J.W. Marriot in Orlando, Florida.
Workshop Description
Dr. Stratman will walk-through the CertLink® MOC program and demonstrate its design, rationale and navigation. According to the ABD, CertLink provides the utmost flexibility in MOC and provides an alternative to the one-time, sit-down, high stakes in-person MOC examination. Dermatologists will be able to go online and take test questions in the convenience of their own home or office at various times throughout the year.
ABD MOC CertLink®
CertLink® is a longitudinal testing platform. The platform is designed to test and build medical knowledge in a “test to competence” type model. In addition, CertLink® will keep dermatologists up to date by providing the latest articles from dermatology subspecialties. CertLink™ assessment platform is powered by American Board of Medical Specialties (ABMS).
Registration and Fees
The pre-conference workshop is provided complimentary for dermatologists registered for ODAC 2020.
About ODAC
Attend ODAC to stay connected, informed, and up-to-date in dermatology. ODAC (previously Orlando Derm) is one of the largest and most prestigious conferences of the year. ODAC attracts a national audience of over 650 US Dermatology Physicians, Dermatology Residents, Nurse Practitioners and Physician Assistants.
Visit orlandoderm.org to register for ODAC and attend this workshop. ODAC is a product of SanovaWorks.

Source: Next Steps in Dermatology
ODAC speaker, Sima Jain, MD provides a two-part series on Hormonal Acne for Next Steps in Derm.
Dermatologists should be able to distinguish which patients presenting with acne may need further evaluation for a possible underlying endocrinopathy. In this two-part series, Dr. Jain will be focuses on hormonal acne specifically related to PCOS, including the exam, work up, diagnosis, treatment and long-term implications of this syndrome.
PCOS is a complex disorder affecting 5-10% of reproductive-age women and is characterized by a state of hyperandrogenism and often hyperinsulinemia. It is the most common endocrine disorder in women and is a major cause of infertility due to lack of ovulation. Patients can present with a wide range of symptoms, which may make the precise diagnosis difficult.
Acne is a common skin manifestation but other potential findings may include hirsutism (increased terminal hairs in a male-pattern distribution, scalp alopecia, acanthosis nigricans and less frequently seborrheic dermatitis. Non-dermatologic symptoms and signs may include irregular menses (oligomenorrhea), insulin resistance, polycystic ovaries and infertility.
Since a dermatologist may be the first or only physician a young female patient with hormonal acne sees, it is imperative for us to be aware of the clinical clues that suggest hyperandrogenism. First, it is important to inquire if the patient’s menstrual cycles are regular to screen for oligomenorrhea and potential anovulation. Be mindful if the patient is on an oral contraceptive pill, as this can mask underlying oligomenorrhea since the external hormones are essentially regulating the menstrual cycle. In addition to discussing the menstrual history, it is important to inquire about potential hirsutism by asking if the patient has noticed increased hair growth to the face (sideburn area, chin, upper cutaneous lip), chest, abdomen and/or inner thighs. Many patients do not realize that increased hair growth may be related to acne and often feel embarrassed to bring it up on their own. A third important feature to be aware of is hair loss to the scalp. It is not uncommon for patients to say they have noticed thinning of their hair or increased shedding, especially to the front of their scalp.
Visit Next Steps in Derm to read the series or attend ODAC to learn more.
